By: Shraddha Srivastava, M3 at A.T. Still University School of Osteopathic Medicine
Reprinted from the fall 2019 issue of The Ohio Family Physician.
In medical school, students are taught the basic ways of managing chronic pain starting with nonsteroidal anti-inflammatory drugs and slowly working their way up to controlled substances. However, we eventually realize that treating chronic pain is no easy feat. There are multiple comorbidities associated with patients, stricter controlled substance laws, and issues with insurance policies that can make any physician feel implicitly overwhelmed and frustrated. With the increasing number of Americans dealing with chronic pain, there needs to be a change in how chronic pain is managed. This article will detail a few non-pharmaceutical methods of treating chronic pain.
As an osteopath, one of the tools we learn is osteopathic manipulative treatment (OMT). These treatments offer a multitude of options for the patient and physician. However, before discussing treatment techniques, it is important to understand the principles leading up to choosing the correct OMT technique.
- The body is a unit; the person is a unit of body, mind, and spirit.
- The body is capable of self-regulation, self-healing, and health maintenance.
- Structure and function are reciprocally interrelated.
- Rational treatment is based upon an understanding of the basic principles of body unity, self-regulation, and the interrelationship of structure and function.
Each principle aims to view the patient as a whole, instead of solely the pains they possess. The different aspects to chronic pain are peripheral trauma, autonomic, myofascial, and viscerosomatic.2 It is important to determine what factors are contributing to the patient’s pain beginning with a head-to-toe examination of key landmarks: the mastoid process; spinal curvature; and inferior angle of the scapula, pelvis, sacrum, and greater trochanters. Each of these landmarks gives the physician an idea of compensatory mechanisms based on the pain. Furthermore, the surrounding tissues in the area can determine the extent to which chronic pain has affected the body. Tissue involving chronic pain tends to feel fibrotic, cool, and dry, and have a decreased range of motion. Based on these observations, a treatment plan using OMT can be devised. However, from an osteopathic perspective, the mind and spirit must also be accounted for. Chronic pain activates the hypothalamic-pituitary-adrenal pathway with constant input to the autonomic nervous system leading to a patient presenting with signs of fatigue, depression, fear of movement, and insomnia.3 Counseling and OMT have proven useful to mitigate the symptoms previously mentioned.
A few techniques that have been proven to be effective in treating chronic pain are Spencer’s technique for shoulder pain, abdominal diaphragm, and myofascial release for back pain; and cranial release for autonomic dysfunction.4, 5, 6 These techniques aim to restore mobility and proper autonomic function.
Spencer’s technique
Use articulatory technique to relieve restriction in the glenohumeral joint. Move the patient’s shoulder through extension (Step 1), flexion (Step 2), circumduction with compression (Step 3), circumduction with traction (Step 4), abduction of shoulder (Step 5), internal rotation (Step 6), and joint pump (Step 7). Bring each motion to the point of resistance and then apply muscle energy (an isometric contraction of muscle against physicians’ force).4
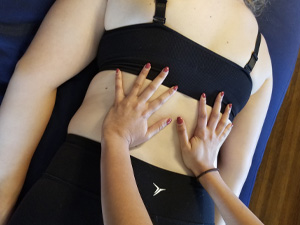
Abdominal diaphragm release
The diaphragm stabilizes the spine during balance and weight-bearing activities. Addressing diaphragm somatic dysfunction can alleviate lower back pain. To release, apply pressure to each side of diaphragm until release of tissue is appreciated.5
Myofascial release
Apply gentle pressure on tissues in the direction of greatest ease. Trauma, inflammatory responses, and/or surgical procedures create myofascial restrictions that can produce tensile pressures of about 2,000 pounds per square inch on pain sensitive structures that do not show up in many standard tests. This technique is beneficial for frail patients, those with osteoporosis, and patients with severe decreased mobility.6
Cranial
The specific cranial technique most studied is the compression of the forth ventricle. This technique is used to restore autonomic response, specifically lowering sympathetic tone, by manipulating the sutures of the skull. In performing this technique, the physician approximates the lateral angles of the occiput. This compresses the fourth ventricle allowing cerebrospinal fluid to flow through natural channels and regulate tissue fluids of the body. Avoid using this technique with patients who have a localized tumor.7, 8
The treatments can be designed in increments over eight weeks, and then scheduled at different intervals for when the patient is in need of an expert. In between these sessions, it is important for the patient to do their part in their treatment plan. Patients can do these techniques and stretches in the comfort of their own home. This allows the patient to be invested in their recovery, while giving them the tools to manage their chronic pain when they are unable to make a visit to their primary care physician. Referring patients to pain specialists or physical therapists, especially underserved patients who tend to have more chronic pain, usually leads to a decreased success rate of treating their pain. Often patients with low social determinants of health have difficulty finding time to make it to their primary care physician, so having a relationship with said patients makes it easier for them to combine OMT treatment with office visits. In the long run, OMT has proven to alleviate chronic pain and improve physician-patient rapport. To learn more about OMT and the positive effects it can have for treating chronic pain.
References available online.




